Case Report
, Volume: 16( 1)Serum Adiponectin and Oxidative Stress Levels in Type 2 Diabetes Mellitus Patients
- *Correspondence:
- Shagufta Hasan
Department of Biochemistry, Andaman and Nicobar Islands Institute of Medical Sciences and Research Centre, Andaman, India
E-mail: annalmedical18@gmail.com
Received: December 30, 2022, Manuscript No. TSBC-23-85117; Editor assigned: January 02, 2023, PreQC No. TSBC-23-85117 (PQ); Reviewed: January 16, 2023, QC No. TSBC-23-85117; Revised: March 02, 2023, Manuscript No. TSBC-23-85117 (R); Published: March 10, 2023, DOI: 10.37532/0974-7427.2023.17(1).178
Citation: Hasan S. Serum Adiponectin and Oxidative Stress Levels in Type 2 Diabetes Mellitus Patients. Biochem Ind J. 2023;17(1):178.
Abstract
Background: Serum adiponectin is a protein that is produced by adipocytes and the kidney. Some recent studies discovered that increased serum adiponectin levels for early detection of nephropathy in Type 2 Diabetes Mellitus (T2DM). This protein has anti-diabetic, anti-oxidative, and anti-inflammatory properties. Increased oxidative stress in T2DM patients causes some micro and macrovascular complications, most notably kidney dysfunction. Estimating serum adiponectin levels may aid in the early detection of nephropathy in T2DM patients, as well as the role of this protein complex. As a result, we planned to look at serum adiponectin rather than urinary micro albuminuria as a predictor of nephropathy in T2DM patients.
Methods: This is a case control study that included 100 T2DM patients divided into two groups based on albumin to creatinine ratio, T2DM patients with normoalbuminuria (N=50) and micro albuminuria (N=50), as well as 50 age and gender matched healthy controls. Urinary albuminuria was determined using the Albumin Creatinine Ratio (ACR), serum adiponectin Enzyme Linked Immunosorbent Assay (ELISA), and serum MDA using the TBARS Method. The mean serum adiponectin levels (8.24 2.36, 19.43 3.08, and 23.94 8.40) in T2DM patients with normoalbuminuria and microalbuminuria, respectively, were significantly higher. Serum MDA levels were also higher in three groups of T2DM patients when compared to healthy controls. Serum adiponectin levels were significantly higher in T2DM with normoalbuminuria compared to T2DM with microalbuminuria and T2DM with micro albuminuria.
Conclusion: Serum adiponectin levels are elevated in T2DM patients with normoalbuminuria, and these levels are linked to renal insufficiency. As a result, this study suggests that adiponectin estimation may be useful for early detection and progression of nephropathy in T2DM patients.
Keywords
Adiponectin; Type 2 diabetes mellitus; MDA; TBARS; Detection
Introduction
Type 2 Diabetes Mellitus (T2DM) is a group of metabolic diseases characterized by hyperglycemia caused by insulin action defects. Hyperglycemia is linked to long term damage, dysfunction and failure of various organs, particularly the kidneys. Poor lifestyle, obesity, ageing, stress and a variety of other factors have all been linked to the disease's prevalence [1,2]. The global prevalence of T2DM is 171 million in 2018, with this number expected to rise to 366 million by 2030. In India, the prevalence is 50.8 million in 2015, rising to 80.0 million by 2030 [3,4]. Nephropathy (DN) is a common and serious microvascular complication of Type 2 Diabetes Mellitus (T2DM). Microalbuminuria is a gold standard and the first clinically available marker for DN [5]. Serum adiponectin is an adipocytokine produced primarily in white adipose tissue but also in kidneys, liver, bones, salivary glands, pancreas and colonial mucosal cells [6]. Adiponectin has anti-diabetic, anti-oxidative and anti-inflammatory properties and it also has renoprotective properties by activating AMP kinase and NADPH oxidase activity [7].
Case Presentation
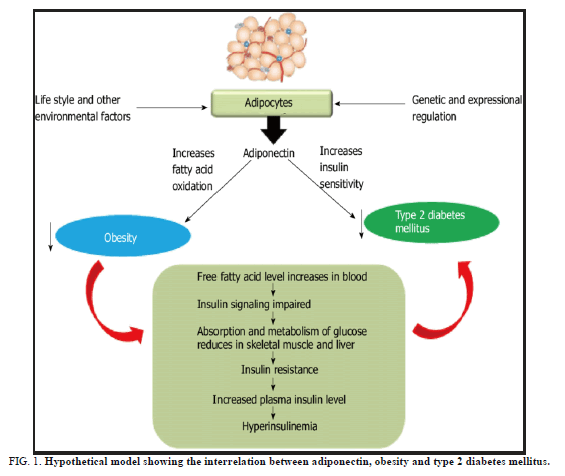
This is a three year case control study at the “Akash Institute of Medical Sciences and Research Centre” in Karnataka. The current study included 150 subjects, 100 of whom were diagnosed with T2DM and aged 30-63 years according to American Diabetes Association (ADA) criteria [8]. The cases are further divided into two groups based on the albumin-creatinine ratio, with 50 T2DM with normoalbuminuria (ACR Ratio: 30 mg/dL) and 50 T2DM with microalbuminuria (ACR Ratio: 30-300 mg/dL) included in the study, as well as 50 age and gender matched healthy controls. After obtaining informed consent and ethical clearance from the institute, all subjects were recruited for the study (IEC no-508). This study excluded patients with a history of hypertension, hypercholesterolemia, cardiovascular disease, hepatic disorders, acute and chronic renal insufficiency, and alcohol abuse. After 12 hours of overnight fasting, five millilitres of venous blood were collected from each patient, with two millilitres transferred into a fluoride tube and three millilitres transferred into a plain tube. The second PPBS sample was collected from all subjects. All of the subjects’ urine was also collected. The collected samples were centrifuged at 3000 rpm for 5 minutes before being stored at -20°C in a deep freezer until biochemical analysis was performed. FBS, PPBS, serum urea, creatinine and uric acid were measured using well established laboratory standard methods; urinary albuminuria was measured using the Albumin Creatinine Ratio (ACR); serum adiponectin was measured using the Enzyme Linked Immunosorbent Assay (ELISA) and serum malondialdehyde was measured using the TBARS method (Figure 1) [9-11].
FIG 1: Hypothetical model showing the interrelation between adiponectin, obesity and type 2 diabetes mellitus.
Statistical analysis
The Kolmogorov Simonov test was used to determine the normal distribution of data. All of the characters are described in detail. For the mean and standard deviation, Microsoft Excel was used. ANOVA was used to determine whether there was a significant difference between the groups of variables. The Pearson correlation was used to determine the relationship between the variables in the study. The data was collected in Microsoft Excel spreadsheets and analyzed with SPSS for Windows version 21.0, with a ‘p’ value of 0.05 considered statistically significant.
Results
The study group’s demographic and biochemical parameters were distributed differently. When compared to healthy controls, plasma fasting blood sugar, postprandial blood sugar, serum urea, creatinine, uric acid, adiponectin and malondialdehyde levels were higher in two groups of T2DM patients. In the current study, a significant difference in the levels of all parameters was observed between two groups of T2DM patients.
Pearson correlation coefficient between variables in the study subjects. Serum adiponectin correlated positively with fasting blood sugar, postprandial blood sugar, serum urea, creatinine, uric acid, urinary albumin and malondialdehyde. Pearson correlation coefficient between variables in the study subjects. Malondialdehyde levels in the blood were found to be positively correlated with plasma fasting blood sugar, postprandial blood sugar, serum urea, creatinine, uric acid, adiponectin and urinary albumin.
Pearson correlation coefficient between variables in the study subjects. Urinary microalbumin levels were found to be positively related to plasma fasting blood sugar, postprandial blood sugar, serum urea, creatinine, uric acid, adiponectin and malondialdehyde levels.
Discussion
Type 2 diabetes mellitus is a chronic metabolic disorder caused by insulin resistance; it may also be caused by improper insulin secretion from pancreatic beta cells. Insulin resistance was caused by beta cells in the pancreas, as well as genetic and metabolic factors [12-14]. Energy production is maintained in this condition by the degradation of lipids and proteins [15]. This process simultaneously generates more free radicals and causes oxidation of polyunsaturated fatty acids, resulting in tissue damage. Malondialdehyde is an oxidative stress biomarker that is produced by lipid peroxidation and other oxidative stress molecules such as acrolein, 4-Hydroxynonenal (HNE), 4-Oxononenal (ONE) and isolevuglandins [16]. The current study discovered that both groups of type 2 diabetes mellitus had elevated levels of serum MDA, indicating that hyperglycemia is also one of the triggering factors for the generation of oxidative stress molecules. Similarly, previous studies discovered that serum MDA levels in type 2 diabetes mellitus patients were positively correlated with HbA1C and that poor glycemic control and advanced drug effects cause micro and macrovascular complications.
Adiponectin is a hormone that is produced primarily by adipose tissues and other tissues such as the liver, kidney, skeletal muscles, bones, salivary glands and so on. The physiological actions of adiponectin in diabetes mellitus play an important role in stimulating the synthesis of insulin production and activation through its anti-diabetic properties, as well as preventing the generation of oxidative stress molecules through its anti-oxidative properties and protecting tissues from inflammation through its anti-inflammatory actions. The current study also compared serum adiponectin levels in type 2 diabetes mellitus patients to healthy controls. Serum adiponectin levels are higher in type 2 diabetes mellitus microalbuminuria than in type 2 diabetes mellitus normoalbuminuria.
Conclusion
FBS, PPBS, urinary microalbumin and serum MDA were all positively correlated with serum adiponectin. Other studies have found that increased serum adiponectin levels in type 2 diabetes mellitus improve glycemic control and protect internal organs from oxidants and inflammatory molecules. Because of its anti-diabetic, anti-oxidant and anti-inflammatory properties, serum adiponectin levels may be useful for early detection of type 2 diabetes mellitus and its complications, according to the current study.
References
- Lakota K, Wei J, Carns M, et al. Levels of adiponectin, a marker for PPAR gamma activity, correlate with skin fibrosis in systemic sclerosis: Potential utility as biomarker?. Arthritis Res Ther. 2012;14(3):1-6.
[Crossref] [Google Scholar] [PubMed]
- Saliba J, Kasim NR, Tamboli RA, et al. Roux-en-Y gastric bypass reverses renal glomerular but not tubular abnormalities in excessively obese diabetics. Surgery. 2010;147(2):282-287.
[Crossref] [Google Scholar] [PubMed]
- Rodríguez-Iturbe B, Garcia GG. The role of tubulointerstitial inflammation in the progression of chronic renal failure. Nephron Clin Pract. 2010;116(2):81-88.
[Crossref] [Google Scholar] [PubMed]
- Sasaki S, Inoguchi T. The role of oxidative stress in the pathogenesis of diabetic vascular complications. Diabetes Metab J. 2012;36(4):255-261.
[Crossref] [Google Scholar] [PubMed]
- Coelho M, Oliveira T, Fernandes R. State of the art paper biochemistry of adipose tissue: An endocrine organ. Arch Med Sci. 2013;9(2):191-200.
- Lilja M, Rolandsson O, Norberg M, et al. The impact of leptin and adiponectin on incident type 2 diabetes is modified by sex and insulin resistance. Metab Syndr Relat Disord. 2012;10(2):143-151.
[Crossref] [Google Scholar] [PubMed]
- Saad EA, Habib SA. Effect of crude extracts of some medicinal plants on the osmotic stability of human erythrocytes in vitro. J Free Radic Antioxid. 2013;139:265-272.
- American Diabetes Association. Economic consequences of diabetes mellitus in the US in 1997. Diabetes care. 1998;21(2):296-309.
- Mancino R, Di Pierro D, Varesi C, et al. Lipid peroxidation and total antioxidant capacity in vitreous, aqueous humor and blood samples from patients with diabetic retinopathy. Mol Vis. 2011;17:1298-1304.
[Google Scholar] [PubMed]
- Nakhjavani M, Esteghamati A, Nowroozi S, et al. Type 2 diabetes mellitus duration: An independent predictor of serum malondialdehyde levels. Singapore Med J. 2010;51(7):582-585.
[Google Scholar] [PubMed]
- Teodoro JS, Nunes S, Rolo AP, et al. Therapeutic options targeting oxidative stress, mitochondrial dysfunction and inflammation to hinder the progression of vascular complications of diabetes. Front Physiol. 2019;9:1857.
[Crossref] [Google Scholar] [PubMed]
- Szaflik JP, Rusin P, Zaleska-Zmijewska A, et al. Reactive oxygen species promote localized DNA damage in glaucoma-iris tissues of elderly patients vulnerable to diabetic injury. Mutat Res. 2010;697(1-2):19-23.
[Crossref] [Google Scholar] [PubMed]
- Rubio-Martin E, Soriguer F, Gutierrez-Repiso C, et al. C-reactive protein and incidence of type 2 diabetes in the Pizarra study. Eur J Clin Invest. 2013;43(2):159-167.
[Crossref] [Google Scholar] [PubMed]
- Sans S, Padro T, Tuomilehto J, et al. Incidence of diabetes and serum adipokines in Catalonian men: The adipocat study. Ann Med. 2013;45(1):97-102.
[Crossref] [Google Scholar] [PubMed]
- Julia C, Czernichow S, Charnaux N, et al. Relationships between adipokines, biomarkers of endothelial function and inflammation and risk of type 2 diabetes. Diabetes Res Clin Pract. 2014;105(2):231-238.
[Crossref] [Google Scholar] [PubMed]
- Sharma R, Satyanarayana P, Anand P, et al. Adiponectin level association with MDA in the patients with type 2 diabetes mellitus. Biomed Pharmacol J. 2020;13(2):943-955.